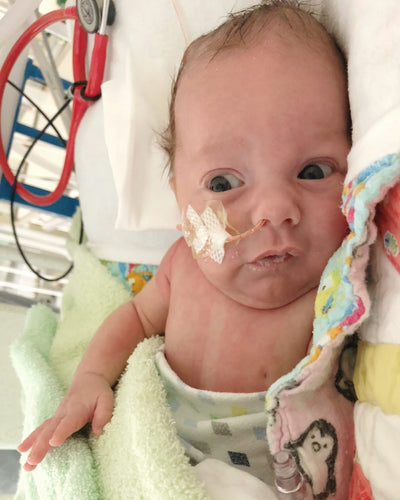
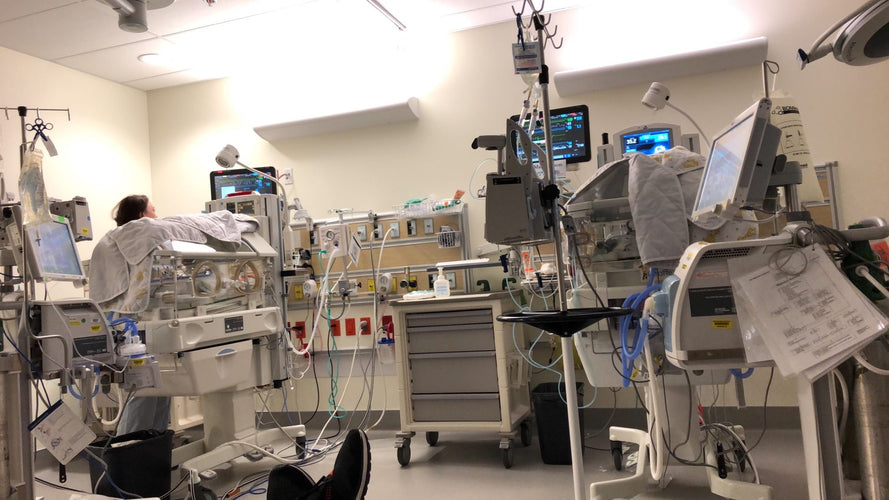
We’ve been home for the same amount of time the boys spent in the NICU now (5 months), so it’s about time I finally got around to writing out Axel’s NICU story!
Axel has always been a fighter, from the womb to the outside. Born at just 1.9lbs at 27 weeks gestation with his brother, Axel was the donor twin in the boys’ Twin to Twin Transfusion Syndrome. This means he was giving away all his blood/nutrients/”STUFF” to his brother and not having enough for himself. (If you’re not sure what TTTS is, you can read more about it here.)
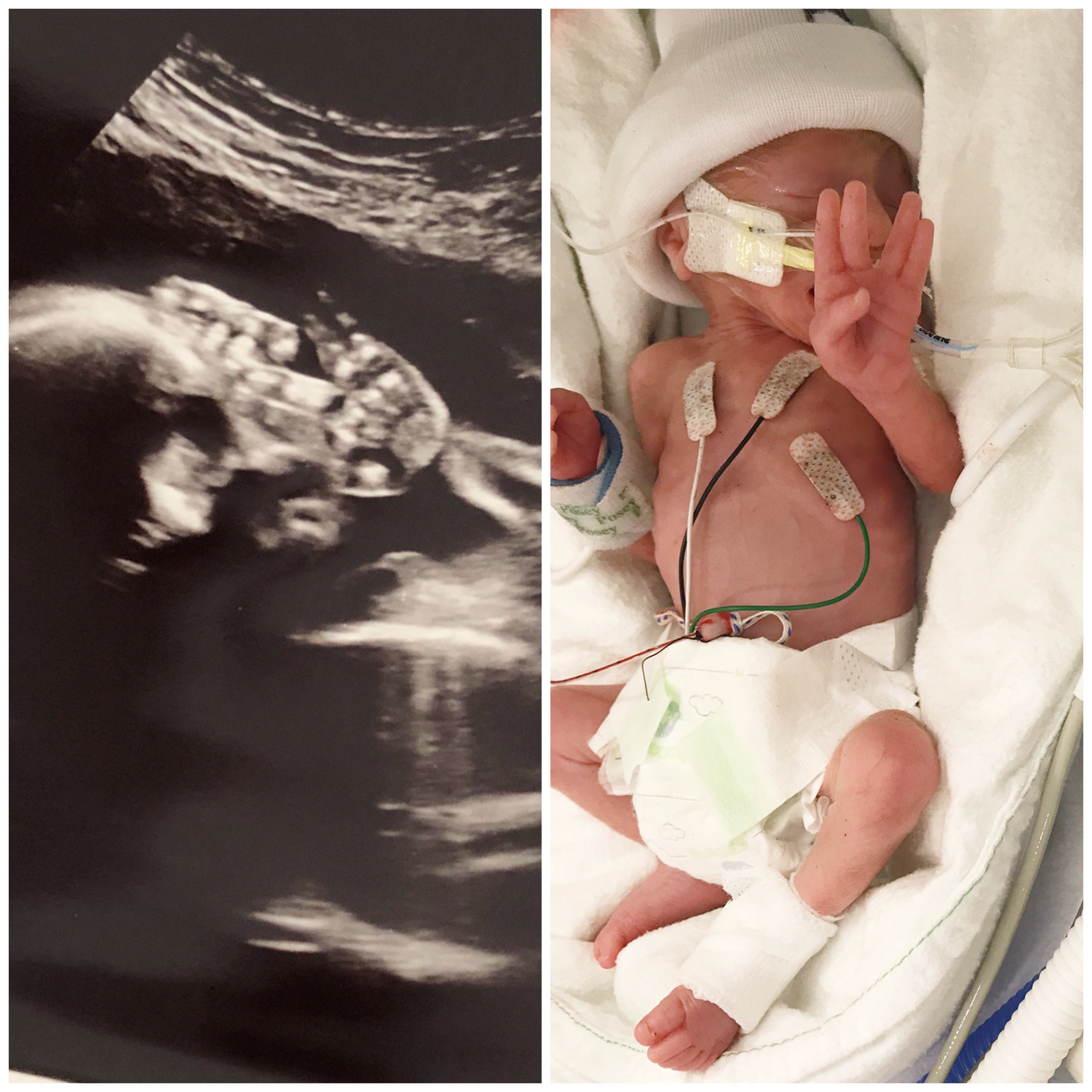
He was much smaller than his brother, who was 2.9lbs at birth. Axel was only 1.9lbs and had very underdeveloped lungs for a 27 weeker. This is likely because he spent over a month with hardly any amniotic fluid, being “stuck” in the intertwin membrane, what is accurately called being a “stuck twin” in TTTS. (My MFM described it as being wrapped in Saran Wrap.)


While both were intubated after birth, Axel spent the longest on respiratory support and has much more severe chronic lung disease than Jaxon. He spent a total of almost 8 weeks intubated and another 5 on CPAP and high flow oxygen support. He finally came off all oxygen 4 days before his due date. 🙂
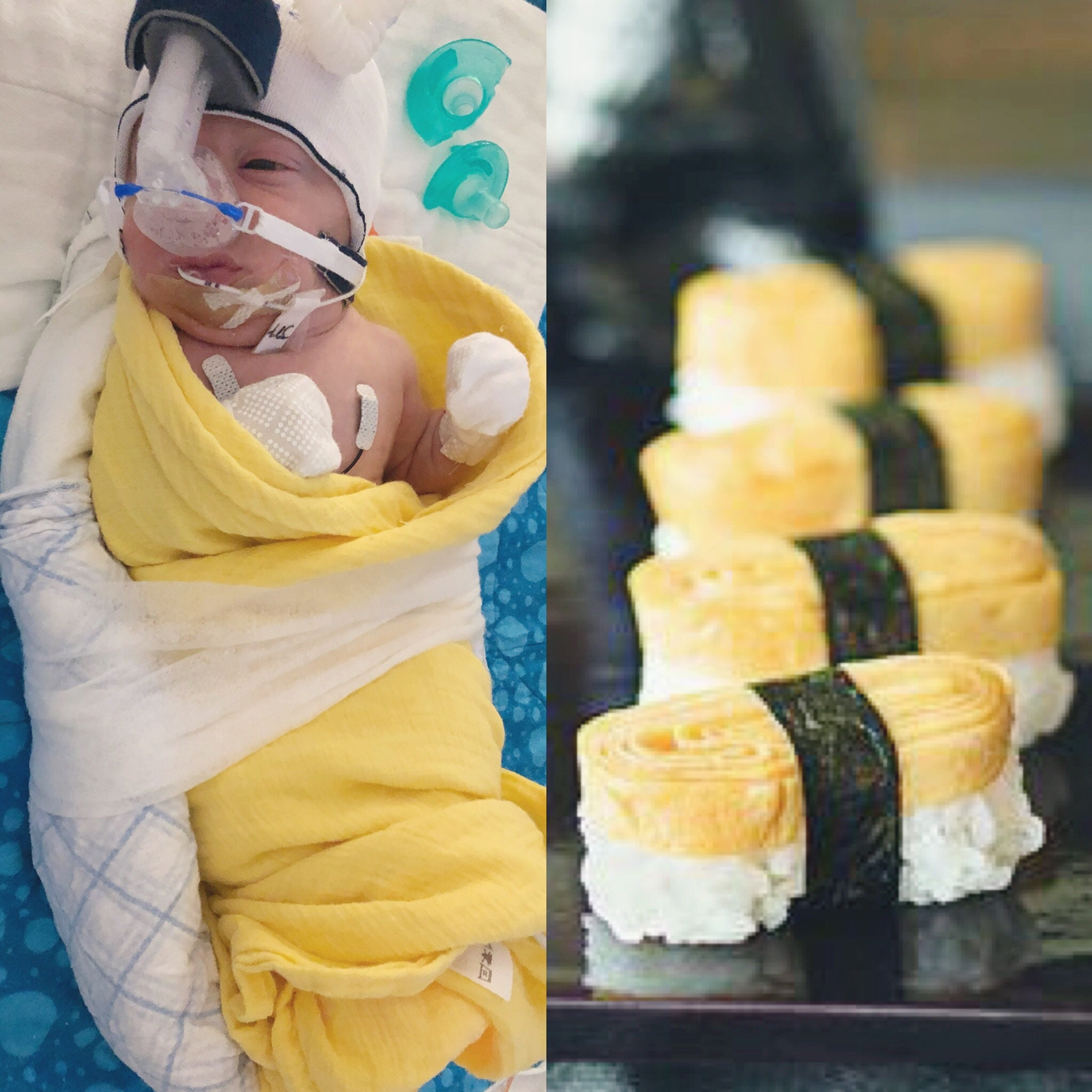
We like to call Axel our little Houdini because he’s escaped a lot of issues.
They told us he would most likely come home on oxygen and need it for up to a year or two of age. But, nope! Kicked it 4 days before his due date.

He had a PDA (open valve in heart) when born and we were told he would likely need surgery for it, but nope! It closed on its own with Tylenol treatment.
We were told he would most likely need a shunt for his hydrocephalus (like bro Jaxon), but so far he has avoided that too and is shunt-free (but continues to be followed closely by neurosurgery in case anything changes and he needs one).
He was close to needing a trach to get off the vent, but luckily a second round of steroid treatment worked to get him from the oscillator to conventional, then finally to NIV and CPAP. We were still told he would probably need oxygen at home, but he never has.
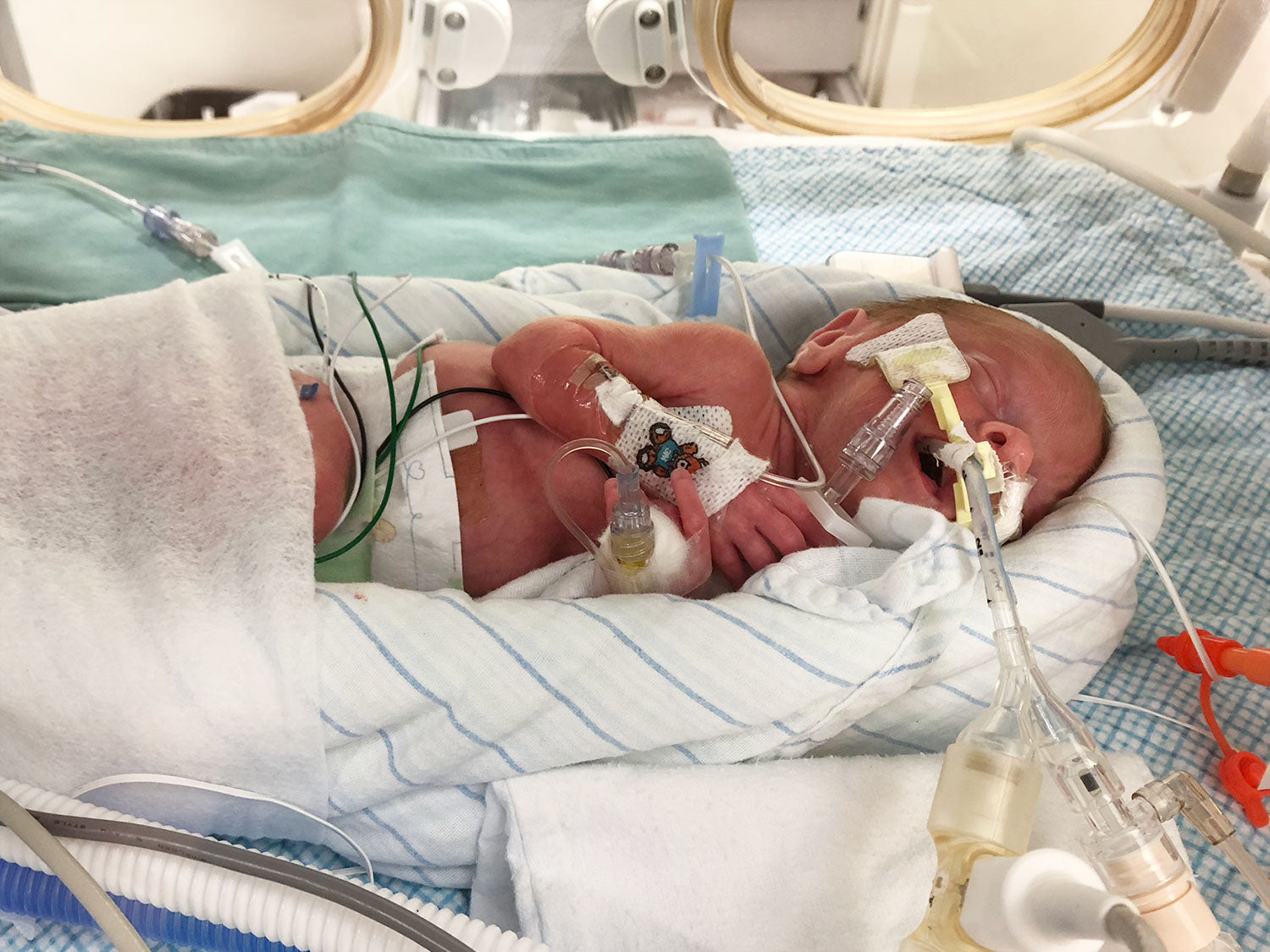
We were told he would never eat on his own. Just before leaving the NICU, he took all his bottles for almost 3 weeks. We were so excited. However, after his eye surgery and a brief re-intubation, he developed a severe aversion and would not eat anything by mouth. He never took a full bottle again after that. We left the NICU with an NG tube, hoping he would go back to eating by mouth, but after a month of no progress, it became clear he wouldn’t. We went ahead with a G-tube in October 2018 and it really was the best choice for him.

He is still mostly G-tube fed now, 10 months later, but we are just starting to try real foods with him and so far, he seems to love it! He’s definitely overcome his aversion issues, so now it’s just about actually learning to eat.
Axel also had ROP (retinopathy of prematurity) like his brother, and required both Avastin injections and laser eye surgery. Thankfully his result was successful and he has normal vision now! We just had his 6 month corrected eye exam. He may have lost some peripheral vision from the surgery (as it does destroy some visual field as a side effect), but it should be minor and so far, he has passed all vision tests with flying colours.
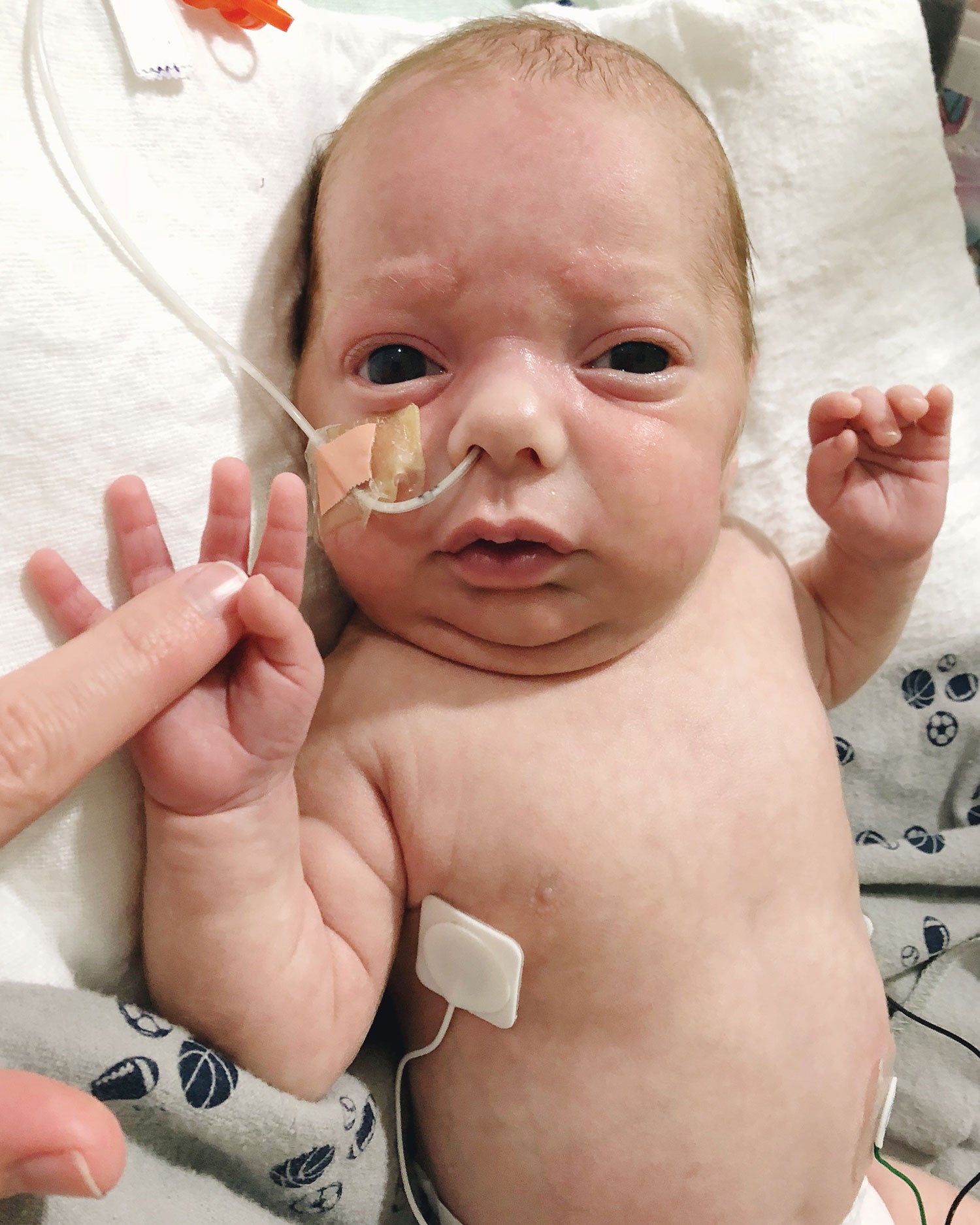
He developed pneumonia twice, failed extubation twice, and several times we were told he may not make it through the night and that he was “unstable.”
He was always very active and actually caused a lot of damage. He pulled out his breathing tube and had to be bagged, pulled out IVs, you name it. He was placed on sedation to curb these activities, though regular morphine didn’t work for him and he needed a cocktail of presidex and a high dose of morphine (for his size) to stay calm.
He was also paralyzed (on purpose) three times when he would not settle and was causing a lot of damage to himself. He caused an internal bleed from moving too much as the breathing tube was moving around his throat/lungs and red blood would come up the tube, showing the presence of internal bleeding. Not good.
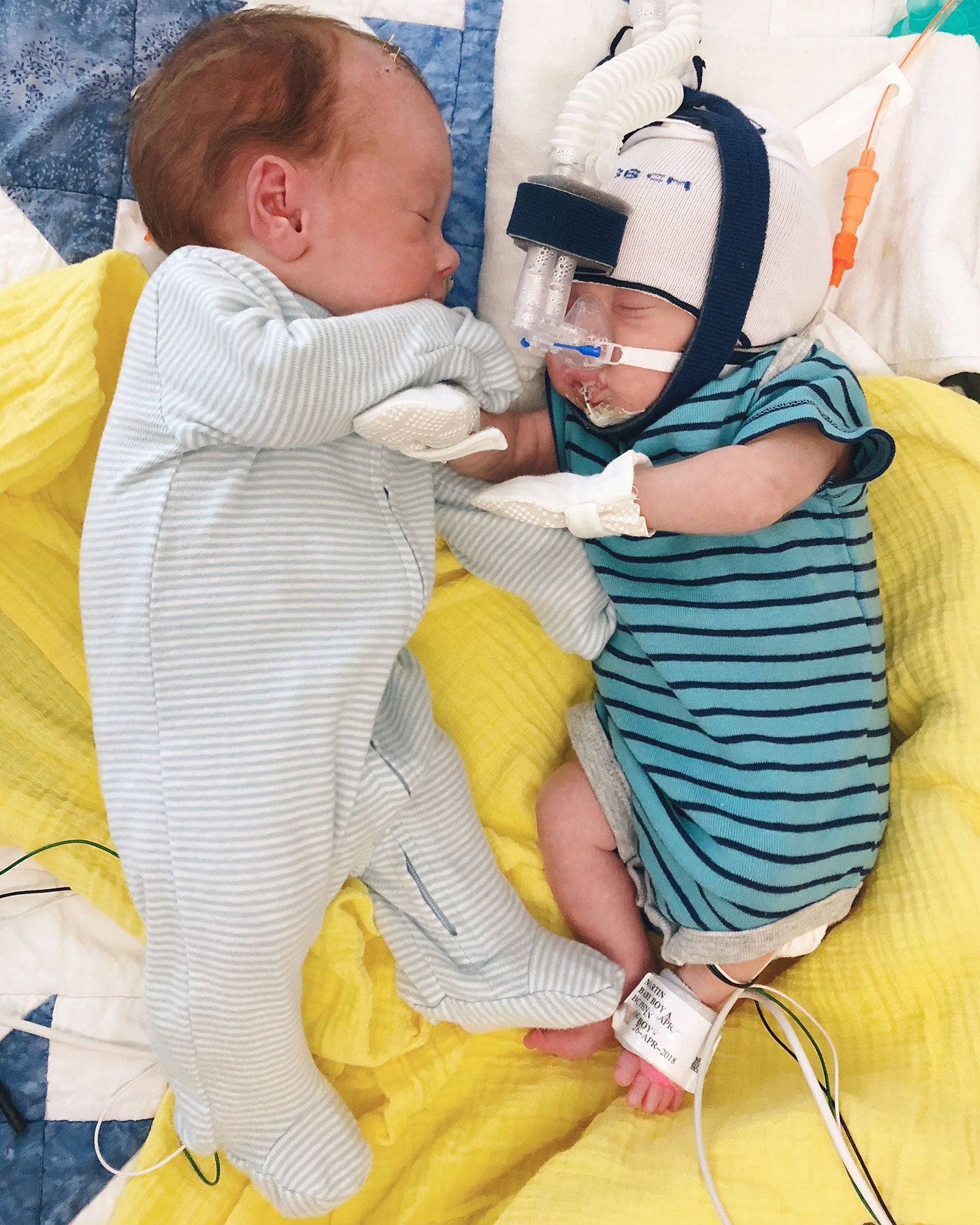
We joked that he was a feisty baby, and he was, already having to fight to survive with not enough nutrients the whole pregnancy being the donor twin. But it was serious too. His brain bleed, a bilateral 4 and first and then downgraded to a 3 on one side and a 4 on the other (not much better), coupled with his respiratory needs and unsettled, possibly seizure-like behaviour, was explained to us as not good…
Scans never confirmed seizures so it’s unknown if he actually had any. But, his future didn’t look too bright. We were offered palliative care for him as well, like Jaxon. We easily could have left the hospital with 0 babies. But we chose to persevere…
And now? Other than his severe reflux still and vomiting, he could almost pass for a regular 6 month old. He is behind in motor milestones, and has some pretty severe tightness in his right arm, which prevents him from fully pushing up in tummy time still and things like that. But, he’s almost met all milestones (except sitting) for his corrected age which is INSANE considering he has a severe brain injury, PVL and was born at under 2lbs, anemic and with an Apgar score of 1.

Now he’s a very giggly, happy and squirmy baby who is curious about everything with a smile that lights up the room (and farts that do too, if a match was lit).
It’s sometimes hard to see his progress compared to Jaxon’s. We don’t compare them to each other, but just in general. We wish Jaxon could see like Axel and experience the world the same way… but we don’t know how the future looks for either of them. Maybe Axel’s muscle tone in his right arm will never go away and he’ll have cerebral palsy on his right side (or both).
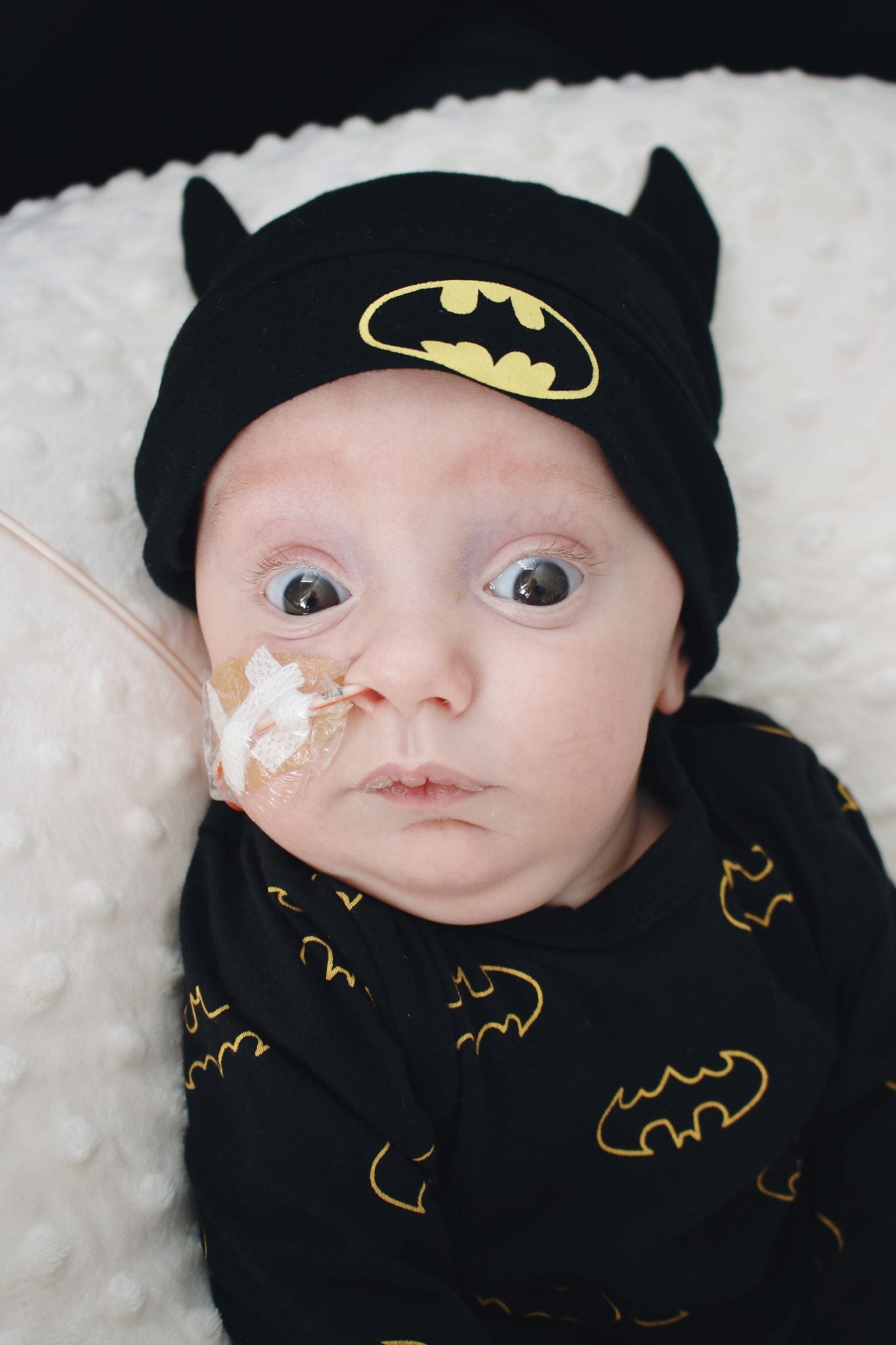
For now, we are so amazed by Axel’s progress and so are all his doctors!
Here’s hoping that progress continues for both boys.